First Seizures
· This addresses patients who, on first assessment, do not appear to have a clear precipitant for their seizure
· For general workup of all seizures see Seizures
Epidemiology and Prognosis
• NEJM study:
o Note that most patients (~75%) were started on medication after the first seizure
o Overall risk of a second seizure was 36% in this setting.
o Remote symptomatic seizure had a much higher risk of recurrence than idiopathic seizures (64% vs 87%)

• Other studies
o Show rate closer to 45-50% (populations with less initial medication prescription)
o FIRST trial – 42% in untreated (see below)
Classification
Seizure type
|
|
Clinical |
Clinical +EEG |
Clinical+EEG+MRI |
|
Classified |
47% |
77% |
81% |
|
Generalized |
8% |
23% |
23% |
|
Partial |
39% |
54% |
58% |
|
Unclassified |
53% |
23% (-30%) |
19% |
·
Note that first EEG yield is higher in children
than adults (39% vs 59%)
Investigations
• See classification (above) for overall success of investigations in classification.
EEG
Data from King et al. 1998:
· Initial EEG epileptiform in 43% of patients
· If non-diagnostic EEG and referred for sleep-deprive EEG – 35% epileptiform
· Total EEG/sleep-deprived EEG – 61% epileptiform
· Timing – early (<24hr) 51% epileptiform vs late (>24hr) 34% epileptiform
§ Suggests greater pick-up rate with early EEG, however other studies have not found such a similar difference.
Predicting recurrence:
· Very little data
· Focal abnormalities seem to have higher risk of recurrence than generalised
· Remote symptomatic seizures with abnormal EEG hold very high risk of recurrence.
Imaging
· Yield for epileptogenic lesion:
|
Total |
14% |
|
Patients presumed focal |
17% |
|
Patients presumed
generalized |
2% |
|
Patients initially
unclassified |
18% |
|
|
|
RMH MRI study 2013
• 764 patients who had MRI as part of first seizure clinic between 2000 and 2009
• Abnormal scan – 45%
• Potentially epileptogenic lesion identified – 23%
• Types of epileptogenic lesions
o Gliosis/encephalomalacia (48%) – mainly stroke, trauma or previous surgery
o Developmental abnormality (15%)
o Vascular anomaly (15%)
o Tumour (15%) – (57% of which were meningioma’s, 23% were glioma’s)
o Mesial temporal sclerosis (8%)
• Yield (i.e. epileptogenic lesion found) according to syndrome:
o Focal - 56%
o IGE – 8%
o Unclassified – 2%
• Reference: Hakami et al. 2013 Neurology 81: 920
Treatment
Should treatment be started after first seizure?
• FIRST trial
o Randomized within one week of first GTCS
o Immediate treatment – 24% relapse at 2yr
o Delayed treatment – 42% relapse at 2yr
- Delayed treatment patients were started on medication after relapse
o At end of 3 years similar numbers had achieved ‘seizure freedom’ with either strategy
- One year seizure freedom (87% vs 83%, immediate v delayed)
- Two year seizure freedom (60% vs 59%, immediate v delayed)
• MESS trial
o Patients for whom there was uncertainty about treatment
o Immediate treatment – 32% relapse at 2yrs
o Delayed treatment – 39% relapse at 2yrs
What medication?
See also Anticonvulsants
|
|
Tonic-Clonic |
Partial |
Absence
|
Atypical* |
|
First-line |
Valproic acid Lamotrigine (child bearing women) |
Carbamazepine Phenytoin Lamotrigine Valproic
acid |
Valproic
acid Ethosuximide |
Valproic
acid |
|
Alternatives |
Phenytoin Carbamazepine Topiramate Zonisamide Felbamate Primidone Phenobarbital |
Topiramate Levetriacetam Tiagabine Zonisamide Gabapentin Primidone Phenobarbital |
Lamotrigine Clonazepam |
Lamotrigine
Topiramate Clonazepam Felbamate |
|
Avoid |
Ethosuximide
Tigabine Vigabatrin |
|
Phenytoin Carbamazepine Tigabine Vigabatrin |
|
* Atypical absence, myoclonic, atonic
Evidence for treatment options
Combined focal and generalised
• LaLiMo Trial (JNNP 2012)
o 400 patients randomised to LTG 200mg or LEV 2000mg
o ~50% focal, ~35% generalised, ~15% undefinable
o Assessed at 6 weeks and 26 weeks
o No significant difference in outcomes
o Trend towards slightly better seizure control with LEV
o Trend towards better tolerability and retention rate with LTG
Focal
• SANAD trials – Arm A – focal seizures
o Recruited patients for whom carbamazepine would have been deemed the best treatment and randomised to alternatives.
o Two major outcomes
- Time to treatment failure (i.e. stopping drug or adding other drugs)
- Achievement of 12months seizure freedom
o In general terms
- Carbamazepine had the best seizure control with Lamotrigine a close second.
- All the other medications had a better side effect profile – except for topiramate
- Lamotrigine had the lowest rate of overall treatment failure.
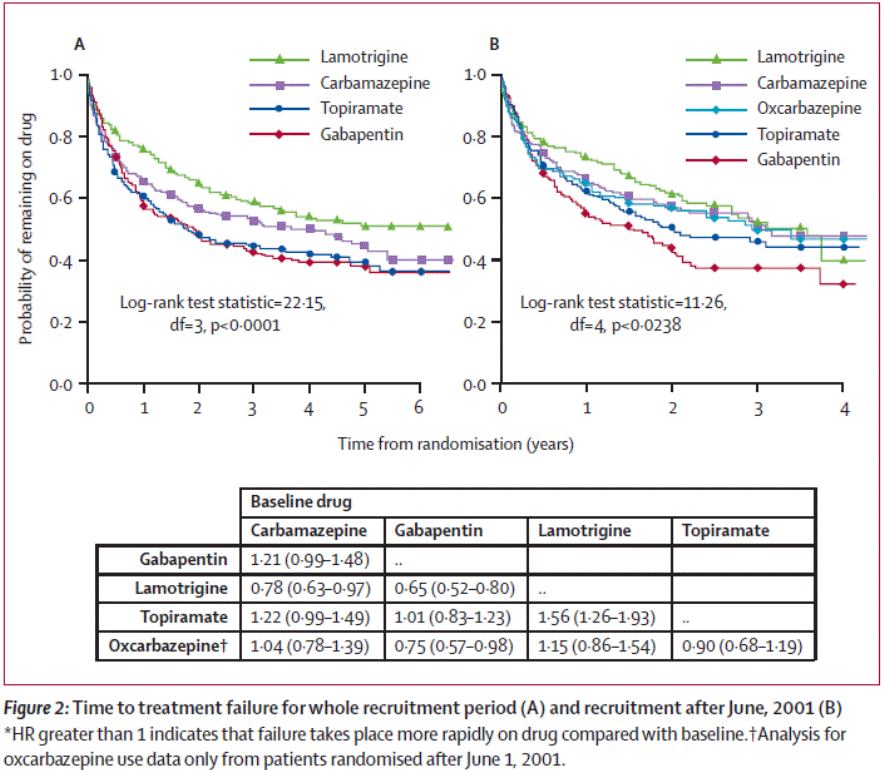

Generalised
• SANAD arm B – generalised seizures
o Patients whom were deemed most suitable for valproate were randomised to other medications
o Outcomes as for SANAD A above.
o In general terms:
- Lamotrigine has slightly better side effect profile (3-5% less failure) but much worse seizure control (15% less) than valproate
- Topiramate has significantly worse side effects (10% more failure) and slightly worse seizure control (~5%) than valproate.


SANAD at 4 years:
|
|
Adverse effect failure % |
Inadequate control % |
Still on drug % |
|||
|
|
Focal |
Gen |
Focal |
Gen |
Focal |
Gen |
|
CBZ |
31 |
|
18 |
|
50 |
|
|
GAB |
20 |
|
39 |
|
39 |
|
|
LTG |
20 |
14 |
24 |
31 |
54 |
50 |
|
TPX |
31 |
29 |
25 |
21 |
42 |
49 |
|
OXC |
26 |
|
24 |
|
49 |
|
|
VPA |
|
21 |
|
16 |
|
60 |
|
|
|
|
|
|
|
|